Best Skincare Routine for Acne-Prone Skin
July 30, 2025
Common Signs of Osteoarthritis in Knees: What You Should Know
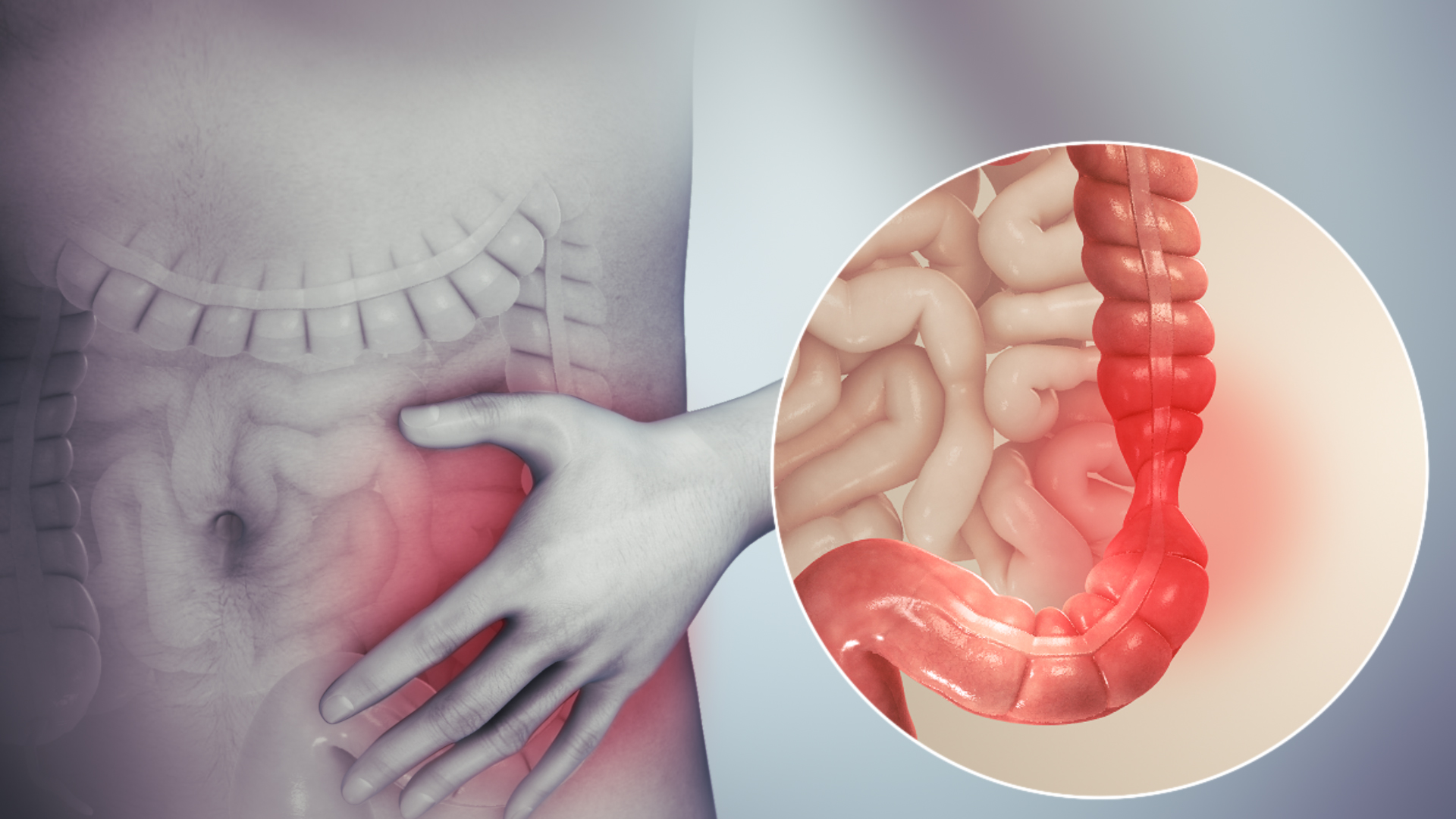
July 30, 2025Irritable Bowel Syndrome, commonly known as IBS, is a long-term condition that affects the digestive system, particularly the large intestine. It’s not a life-threatening illness, but it can be very uncomfortable and have a big impact on your daily life. Many adults live with IBS without even realizing what’s causing their stomach troubles. This article will explore the main symptoms of IBS in adults, how it feels, why it happens, and what you can do about it.
What is Irritable Bowel Syndrome (IBS)?
IBS is a functional gastrointestinal disorder. This means that the digestive system looks normal in tests, but it doesn’t work properly. IBS is more common in adults, especially women, and tends to appear between the ages of 20 and 50. The exact cause isn’t fully known, but it is often linked to stress, food sensitivities, infections, or changes in gut bacteria.
Common Symptoms of IBS in Adults
Let’s dive into the typical symptoms experienced by adults with IBS. These symptoms can vary from person to person and may come and go over time.
1. Abdominal Pain and Cramping
The most common symptom of IBS is pain in the belly. This pain can feel dull or sharp and usually gets worse after eating. It might improve after you go to the bathroom. The discomfort is often felt in the lower part of the abdomen and can last from a few minutes to several hours.
2. Bloating and Gas
People with IBS often complain of feeling bloated or full, even after eating small meals. This happens due to excess gas in the digestive system. Your stomach may look swollen, and you may feel uncomfortable wearing tight clothes.
3. Changes in Bowel Habits
IBS affects how often you go to the bathroom and the texture of your stool. Some people experience:
- Diarrhea (IBS-D): Frequent loose or watery stools.
- Constipation (IBS-C): Difficulty passing stools or fewer bowel movements.
- Mixed type (IBS-M): Alternating between diarrhea and constipation.
This unpredictable change in bowel movements can be very frustrating for those dealing with IBS.
4. Mucus in Stool
Another sign of IBS is the presence of white or clear mucus in your stool. While mucus is normal in small amounts, seeing it often or in large amounts might indicate IBS.
5. Urgency and Incomplete Bowel Movements
Many adults with IBS feel a strong urge to go to the bathroom suddenly, especially after eating. You might also feel like you haven’t fully emptied your bowels, even after going.
6. Fatigue and Sleep Issues
IBS doesn’t just affect the gut — it can also lead to tiredness and poor sleep quality. Many people report feeling exhausted, even after a full night’s sleep, likely due to the discomfort and stress caused by IBS.
7. Nausea and Appetite Changes
Some adults with IBS feel nauseated, especially after eating certain foods. This can affect your appetite and lead to unintentional weight loss if not managed properly.
8. Anxiety and Depression
Living with IBS can affect your mental health. The ongoing discomfort, unpredictability, and embarrassment associated with the condition can lead to anxiety and depression. In fact, there is a strong connection between the brain and gut — sometimes called the “gut-brain axis.”
Less Common but Possible Symptoms
Though not everyone experiences them, some additional symptoms might include:
- Back pain
- Frequent urination
- Headaches
- Bad breath (due to poor digestion)
- Heartburn or acid reflux
Triggers of IBS Symptoms
IBS symptoms can be triggered or worsened by several factors:
- Diet: Spicy foods, caffeine, dairy, and high-fat meals can set off symptoms.
- Stress: Emotional stress is a major trigger for many adults.
- Hormones: Women may notice worse symptoms around their menstrual cycle.
- Infections: A past stomach infection can increase the risk of IBS.
When to See a Doctor
While IBS is not life-threatening, some symptoms can overlap with other serious digestive diseases. You should see a doctor if you notice:
- Blood in your stool
- Unexplained weight loss
- Severe or sudden abdominal pain
- Symptoms that wake you up at night
These could point to conditions like Crohn’s disease, ulcerative colitis, or even colon cancer.
Diagnosis and Testing
There’s no single test for IBS. Doctors usually diagnose it based on symptoms and by ruling out other conditions. You may undergo:
- Blood tests
- Stool tests
- Colonoscopy (in some cases)
- Imaging like ultrasound or CT scan
Doctors may use the Rome IV Criteria, which looks at specific symptoms over a 3-month period, to help diagnose IBS.
Managing IBS Symptoms
There is no cure for IBS, but it can be managed with lifestyle changes, diet, and sometimes medication. Here’s what can help:
1. Dietary Adjustments
- Low FODMAP Diet: Avoid certain carbs that are hard to digest.
- Increase fiber (for IBS-C).
- Avoid trigger foods like dairy, gluten, caffeine, and processed foods.
2. Stress Management
- Regular exercise like walking or yoga
- Deep breathing or meditation
- Cognitive Behavioral Therapy (CBT) or counseling
3. Medications
- Antispasmodics (for cramps)
- Laxatives (for constipation)
- Anti-diarrheal medications
- Probiotics and digestive enzymes
Living With IBS
IBS is a condition you may have to manage for the long term, but you’re not alone. Millions of adults around the world live full, healthy lives while managing their IBS. The key is to listen to your body, identify your triggers, and make adjustments that work for you.
Frequently Asked Questions (FAQs)
1. Can IBS go away on its own?
IBS is a chronic condition, which means it typically doesn’t go away completely. However, symptoms can improve or disappear for long periods with the right lifestyle changes and treatment.
2. Is IBS dangerous or life-threatening?
No, IBS is not life-threatening and doesn’t cause permanent damage to your intestines. But it can significantly affect your quality of life if left unmanaged.
3. What foods should I avoid with IBS?
Common trigger foods include spicy foods, caffeine, alcohol, carbonated drinks, fatty foods, and dairy. A low FODMAP diet is often recommended to help find and avoid triggers.
4. How is IBS different from IBD (Inflammatory Bowel Disease)?
IBS is a functional disorder with no visible damage to the intestines. IBD, which includes Crohn’s disease and ulcerative colitis, involves actual inflammation and damage to the digestive tract and can lead to serious complications.
5. Can stress really make IBS worse?
Yes, stress plays a major role in worsening IBS symptoms. The gut and brain are closely connected, and emotional stress can trigger physical symptoms in the digestive tract.
Conclusion
IBS is a manageable, though frustrating, condition that affects millions of adults. Recognizing the symptoms — such as abdominal pain, bloating, and irregular bowel habits — is the first step to finding relief. Through healthy eating, stress management, and sometimes medication, you can take back control of your gut and your life.