What to Expect During a Dental Cleaning: A Step-by-Step Guide
July 30, 2025
How to Manage Post-Op Pain After Orthopedic SurgerySimple, Effective, and Human-Friendly Guide
July 30, 2025Joint pain can affect anyone—whether you’re an athlete, an office worker, or simply aging gracefully. The discomfort might stem from arthritis, injuries, overuse, or degenerative conditions. When the pain begins to interfere with your daily life—such as walking, sleeping, or even holding a cup of coffee—you might start looking into treatments.
There are two primary treatment routes: surgical and non-surgical. But how do you decide which one is best for you? Let’s dive into the pros, cons, and comparisons of both, explained in a simple, clear way that helps you make the right choice.
Understanding Joint Pain
Joints are the connections between bones—like your knees, hips, shoulders, and fingers. Over time or due to injury, these joints can wear down or become inflamed, causing stiffness, swelling, and pain.
Common causes of joint pain include:
- Osteoarthritis (wear and tear of cartilage)
- Rheumatoid arthritis (autoimmune inflammation)
- Injury or trauma
- Tendonitis or bursitis
- Overuse or repetitive motion
Non-Surgical Treatments for Joint Pain
Non-surgical (or conservative) treatments are typically the first step in managing joint pain. They are less invasive and focus on reducing inflammation, strengthening muscles, and improving joint function.
1. Physical Therapy
Working with a physical therapist helps improve joint mobility and strengthen the muscles around the joint. Regular sessions can reduce pain, improve balance, and prevent further damage.
Best for: Early-stage arthritis, post-injury recovery, or chronic joint stiffness.
2. Medications
Over-the-counter options like ibuprofen or acetaminophen help reduce inflammation and pain. For more severe cases, doctors might prescribe stronger anti-inflammatory drugs or corticosteroid injections.
Note: Long-term use of medications can have side effects like stomach issues or increased blood pressure.
3. Lifestyle Changes
Losing excess weight, eating an anti-inflammatory diet (rich in omega-3s and vegetables), and staying active can do wonders. Obesity adds extra stress on joints, especially knees and hips.
4. Bracing or Assistive Devices
Knee braces, orthotics, or canes can help support your joints, reduce pressure, and improve mobility.
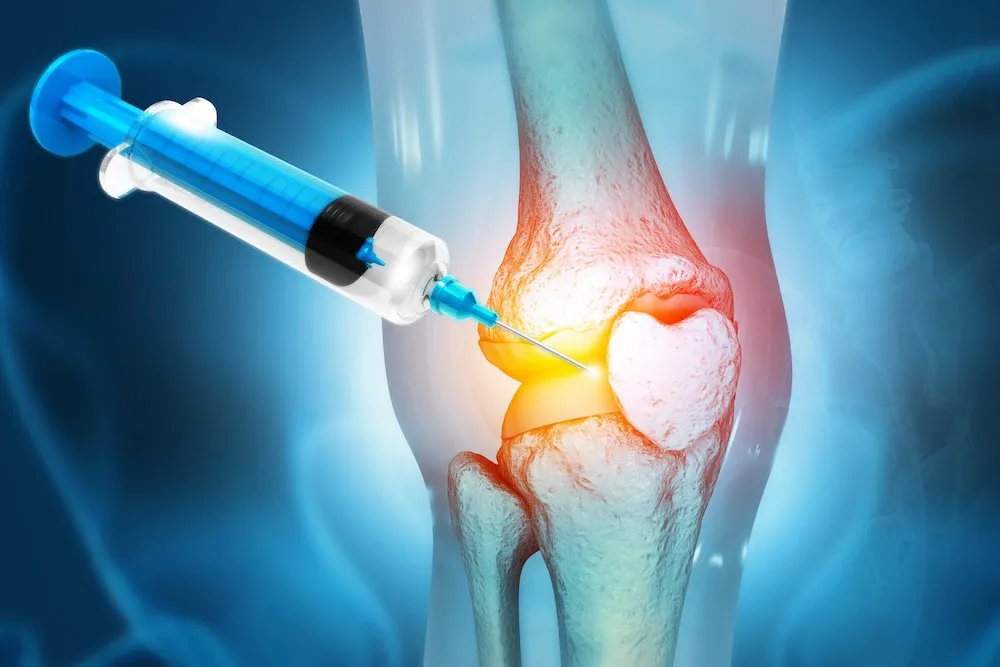
5. Injections
- Corticosteroids: Fast pain relief, but only short-term.
- Hyaluronic acid: Lubricates the joint (often used for knee osteoarthritis).
- Platelet-rich plasma (PRP): Uses your own blood to promote healing.
When is Surgery Needed?
If non-surgical treatments don’t provide enough relief or if your joint is severely damaged, surgery may be the best option. This is often considered when joint pain significantly limits your daily life and movement.
Common Surgical Treatments
1. Arthroscopy
A minimally invasive procedure where a tiny camera is inserted into the joint to repair damage. It’s often used for torn ligaments, meniscus tears, or cartilage damage.
Pros: Smaller incision, faster recovery.
Cons: Not effective for severe arthritis.
2. Joint Replacement (Arthroplasty)
This is more common for hips and knees. The damaged joint is replaced with an artificial implant made of metal, ceramic, or plastic.
Pros: Long-term pain relief, improved quality of life.
Cons: Requires longer recovery and physical therapy.
3. Joint Fusion (Arthrodesis)
In some cases, especially with severe arthritis in the ankle or spine, the joint is fused together to eliminate movement and pain.
Pros: Permanent pain relief.
Cons: Loss of joint mobility.
Surgical vs. Non-Surgical: A Side-by-Side Comparison
| Feature | Non-Surgical Treatment | Surgical Treatment |
|---|---|---|
| Invasiveness | Non-invasive | Invasive |
| Recovery Time | Shorter | Longer (weeks to months) |
| Effectiveness | Good for mild to moderate pain | Best for severe joint damage |
| Risks | Fewer side effects | Infection, blood clots, anesthesia risks |
| Cost | Usually less expensive | Can be expensive, especially without insurance |
| Long-term Solution | Temporary relief | Can be permanent |
How to Decide What’s Right for You
Here are some questions to consider with your doctor:
- How severe is your joint damage?
- Have you tried all non-surgical options?
- Is the pain affecting your quality of life?
- Are you healthy enough for surgery?
- What are your goals—pain relief, better mobility, or both?
Often, doctors recommend starting with non-surgical methods. If these don’t help, surgery may be a logical next step.
FAQs
1. Can joint pain go away without surgery?
Yes. Many people find relief with physical therapy, medications, and lifestyle changes. Surgery is usually a last resort when non-surgical treatments no longer work.
2. How long is recovery after joint surgery?
It depends on the type of surgery. Arthroscopy might take a few weeks, while a full joint replacement may take 3-6 months for full recovery with physical therapy.
3. What are the risks of joint surgery?
Risks include infection, blood clots, nerve damage, or failure of the implant. However, modern surgical techniques have made these complications less common.
4. Are injections a good long-term solution?
Injections like steroids offer short-term relief but are not a long-term fix. Overuse can even damage the joint over time. PRP and hyaluronic acid may offer longer benefits in some cases.
5. When should I see a doctor about joint pain?
If the pain lasts more than a few weeks, affects your daily life, or is accompanied by swelling, stiffness, or reduced range of motion, it’s time to see a healthcare provider.
Conclusion
Joint pain doesn’t always mean surgery. In many cases, non-surgical options like physical therapy, medication, and lifestyle changes can significantly reduce discomfort. However, for those with advanced joint damage or when conservative methods no longer help, surgery can offer a life-changing solution.
The key is to work closely with your doctor, consider your daily needs, and weigh the pros and cons of each approach. With the right plan, relief is possible—and so is getting back to the activities you love.